The most important function of the periodontal ligament is to attach the tooth to the surrounding bone. Another important function is the damping of occlusal forces. Additionally, the periodontal ligament serves as an important reservoir for cells that are constantly needed for tissue homeostasis and play a crucial role in periodontal wound healing and regeneration (periodontal fibroblasts, cementoblasts, odontoclasts, osteoblasts and osteoclasts, epithelial cell rests of Malassez, monocytes and macrophages, and undifferentiated mesenchymal progenitor and stem cells).
The fibroblasts of the periodontal ligament synthesize, structure, and remodel the extracellular matrix, which consists of collagen fibers and an amorphous ground substance composed of non-collagenous proteins. Due to its structural configuration, the periodontal ligament provides a flexible attachment of the tooth to the surrounding bone via Sharpey’s fibers into the mineralized tissues (Nanci and Bosshardt 2006).
Root cementum
Root cementum is a mineralized connective tissue coating the roots of teeth, usually extending from the cementoenamel junction to the root apex. Its primary function is to invest and attach the fibers of the periodontal ligament to the root surface (the acellular extrinsic fiber cementum, AEFC, and the cellular mixed stratified cementum, CMSC). However, root cementum also has other important functions, such as adjusting the tooth position to new physiologic requirements and repair of root defects (cellular intrinsic fiber cementum, CIFC) (Nanci and Bosshardt 2006).
Alveolar bone
The teeth are anchored in the alveolar bone , a part of the alveolar process that consists of an outer cortical plate, an inner cortical plate, and a central spongiosa. The alveolar process is continuous with the jawbone and can only develop in the presence of teeth. The inner cortical plate lines the alveolus and is also referred to as the alveolar bone.
In fully erupted and periodontally healthy teeth, the contour of the alveolar crest follows the contour of the cementoenamel junction in a coronoapical direction for approximately 2 mm (Saffar and coworkers 1997). The alveolar bone consists of compact bone characterized by the presence of osteons, the structural unit for cortical bone remodeling. The socket wall exhibits many perforations that connect the periodontal ligament with the endosteal or bone-marrow spaces, thus enabling blood and lymph vessels, and nerve fibers, to pass through these openings.
A characteristic component of the alveolar bone is the bundle bone , which is deposited in successive layers running parallel to the socket wall. Its typical appearance is determined by the Sharpey’s fibers penetrating its layers. The alveolar bone responds to the functional demands placed on it by the processes of resorption and deposition, known as bone remodeling .
Structure of peri-implant tissues in health
During the process of wound healing following the placement of dental implants, the features of the peri-implant mucosa are established (Sculean and coworkers 2014) (Figs 6 to 10).
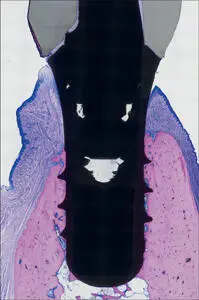
Fig 6 Photomicrograph. Osseointegrated dental implant with direct bone-to-implant contact and supracrestal soft-tissue implant contact.
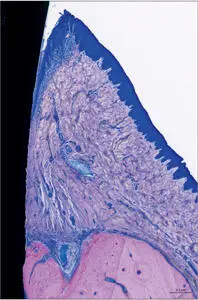
Fig 7 Higher magnification- Supracrestal peri-implant soft tissues consisting of oral and sulcular epithelium and connective tissue adhesion to the implant surface.
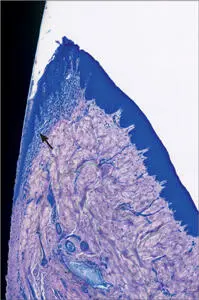
Fig 8 Higher magnification. Coronal portion of the supracrestal peri-implant soft tissues. The oral and sulcular epithelium are clearly visible. The collagen fibers located apically to the junctional epithelium run parallel to the implant surface. A more diffuse inflammatory infiltrate (arrow) is located immediately adjacent the junctional and sulcular epithelium.
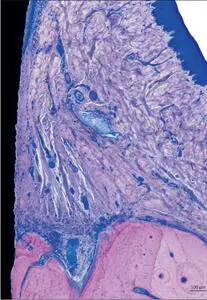
Fig 9 Higher magnification. Supracrestal portion of the peri-implant soft tissues. The collagen fibers located apically to the junctional epithelium run parallel to the implant surface.
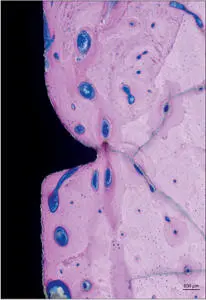
Fig 10 Higher magnification. Direct contact between the bone and the implant surface (osseointegrated implant).
Berglundh and coworkers (1991) examined the anatomical and histological features of the peri-implant mucosa in dogs, formed in a two-stage procedure, and compared these with those of the gingiva around teeth. The peri-implant mucosa consisted of a keratinized oral epithelium located at the external surface, connected to a thin barrier epithelium facing the abutment (the equivalent to the junctional epithelium around teeth), the peri-implant junctional epithelium . It terminated 2 mm apical to the coronal soft-tissue margin and 1.0 to 1.5 mm coronal to the peri-implant bone crest. The mean supracrestal soft tissue (including the sulcus depth) measured 3.80 mm around implants and 3.17 mm around teeth. While there was no statistically significant difference in the height of the junctional epithelium and sulcus depth between implants and teeth, the height of the soft connective tissue was statistically significantly greater around implants than around teeth (Fig 11).
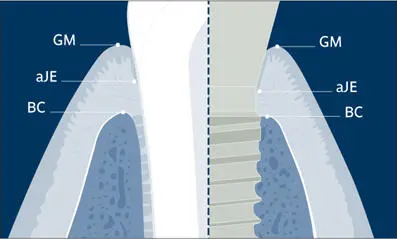
Fig 11 Schematic drawing. illustrating the structure of clinically healthy supra-alveolar soft tissues adjacent to a tooth or an implant (GM: gingival margin, aJE: apical extent of the junctional epithelium, BC: bone crest).
The peri-implant junctional epithelium and the soft connective tissue adjacent to the abutment appeared to be in direct contact with the implant/abutment surface (Berglundh and coworkers 1991). In summary, the findings of this study showed that the peri-implant mucosa displays comparable anatomical features to those of gingiva around teeth (Berglundh and coworkers 1991).
Subsequent studies provided evidence that a similar mucosal attachment is formed on titanium with different implant systems (Buser and coworkers 1992; Abrahamson and coworkers 1996) and around implants placed using both non-submerged and submerged approaches (Abrahamson and coworkers 1999; Arvidson and coworkers 1996; Weber and coworkers 1996). However, the peri-implant junctional epithelium was significantly longer in implants placed using a submerged approach, where an abutment was connected in a second-stage surgical procedure, than in implants placed using a non-submerged approach (Weber and coworkers 1996).
The biologic width (of the supracrestal soft tissue) was revisited in a further dog experiment, following connection of the abutment to the implant with or without a reduced vertical dimension of the oral mucosa (Berglundh and coworkers 1996). It was found that while the peri-implant junctional epithelium was about 2 mm in depth, the supra-alveolar soft connective compartment had a depth of approximately 1.3 to 1.8 mm.
Читать дальше