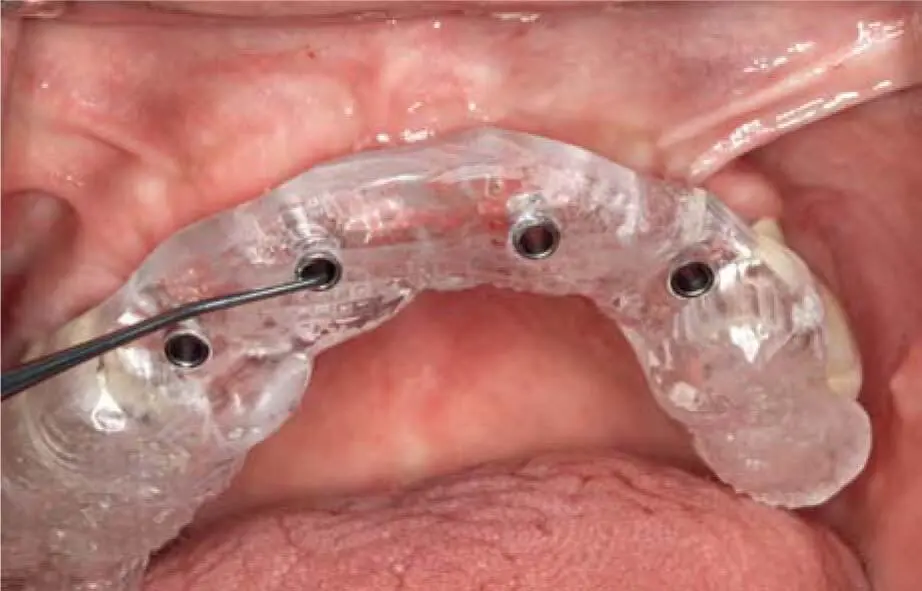
Fig 2-20iUse of a surgical guide at second stage surgery to determine the positions of the implants.
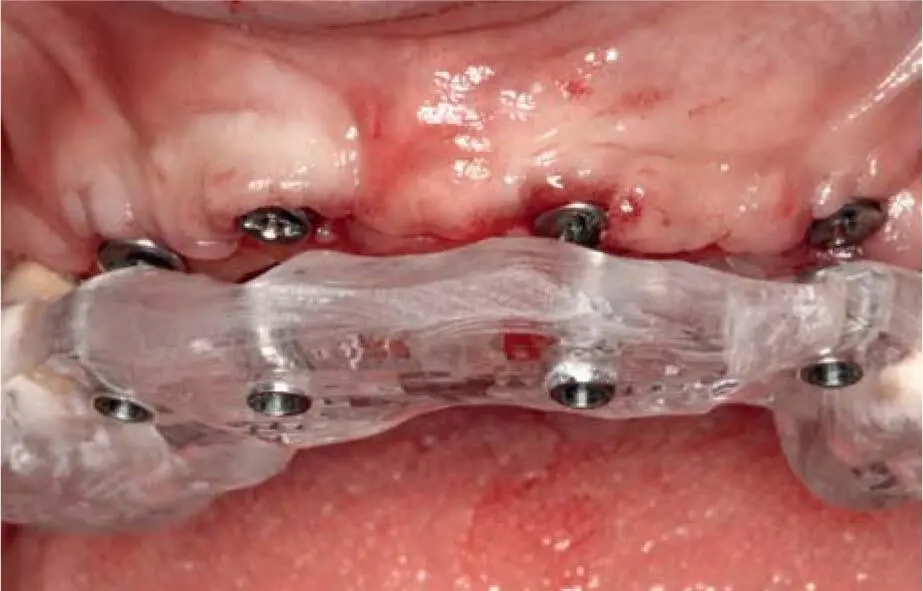
Fig 2-20jControl of implant positions using the surgical guide after insertion of the healing abutment at second stage surgery.
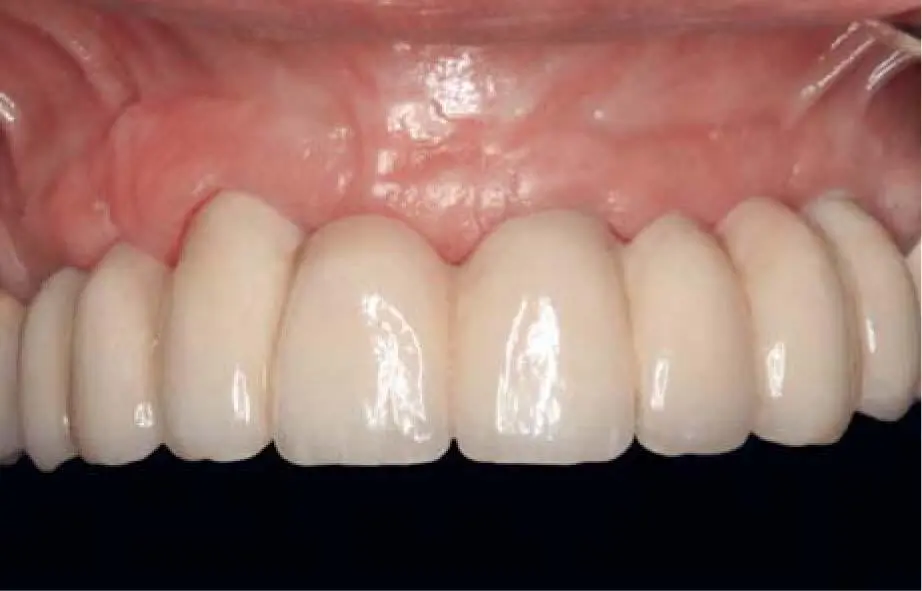
Fig 2-20kDefinitive restoration with stable and healthy soft tissue 2 years postoperatively.
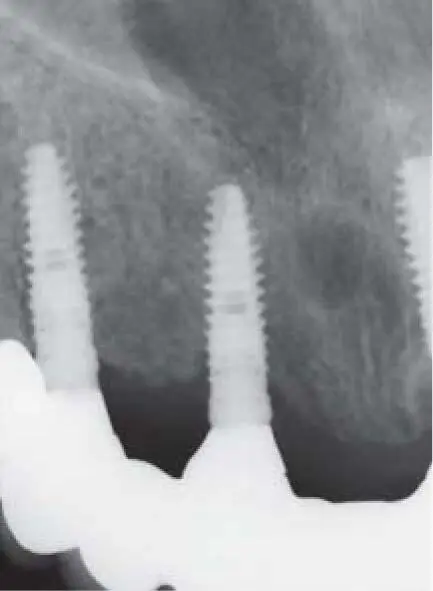
Fig 2-20lRadiographic control of the implants in the right maxilla.
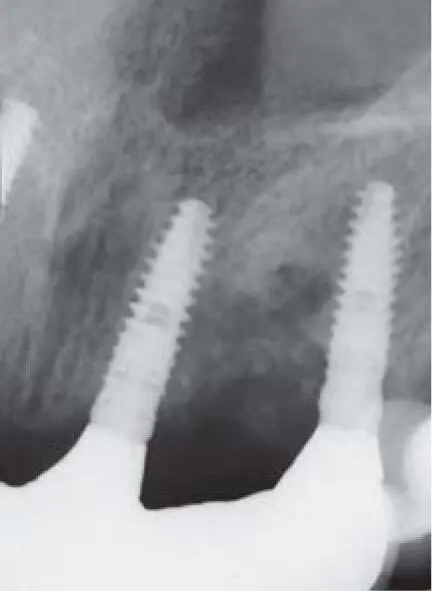
Fig 2-20mRadiographic control of the implants in the left maxilla.
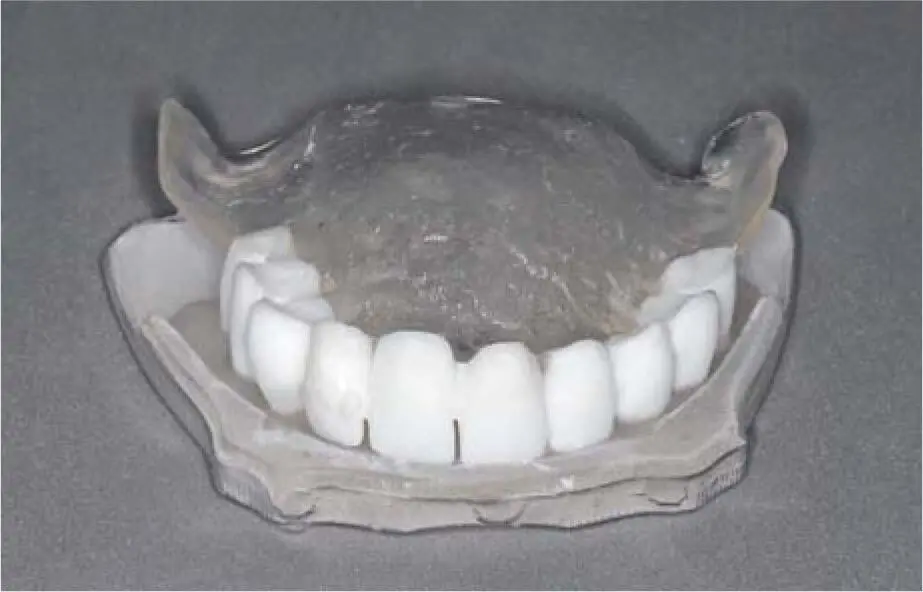
Fig 2-21Tooth-shaped radiologic template for the edentulous maxilla in transparent resin for the base. The clearly separated crowns rest on the base so that the soft tissue configuration can be determined indirectly.
2.5 Choice of grafting technique
The grafting procedure is determined by various factors such as the extent of the bone atrophy, the number of implants necessary for the long-term support of the prosthetic restoration, the maxillomandibular distance, the antagonist dentition, and the soft tissue situation.
Bone grafting procedures are usually not necessary in the presence of a bone volume of > 10 mm vertically and > 7 mm horizontally; however, sometimes due to the soft tissue situation or the planned prosthetic restoration an alveolar crest reconstruction may be required.
The decision regarding which grafting procedure to recommend in a specific clinical situation depends naturally on the defect morphology and the anatomical conditions.
2.5.1.1 Horizontal bone atrophy
If the bone width is partly or completely insufficient, without vertical bone loss in the esthetic region and a remaining vertical bone height of > 10 mm in the other regions, the following procedures are recommended:
 In the case of a partly bony defect on the vestibular and or palatal/lingual bone wall by a remaining crestal bone width of > 6 mm, implants can be inserted in combination with bone grafting using local bone chips and bone cores collected during implant preparation, with or without the membrane technique. 37,49,92However, the decision to use this technique is also strongly determined by the position of the smile line, which may require further grafting to adapt the gingival contour of the adjacent teeth and contour of the peri-implant soft tissue according to the overall esthetic situation. 43The decision about whether implant placement should be performed simultaneously with grafting or after the consolidation of the graft depends on the morphology of the defect and whether the implant can be placed within the jaw contours (see Chapter 4). Bone spreading can play an important role in preserving and expanding the remaining bone by stretching the bone walls of the future implant site, augmenting the chance of implant insertion inside the bony contour. 62If these conditions are not met, it is recommended to first carry out the grafting, and then to insert the implant after 3 months.
In the case of a partly bony defect on the vestibular and or palatal/lingual bone wall by a remaining crestal bone width of > 6 mm, implants can be inserted in combination with bone grafting using local bone chips and bone cores collected during implant preparation, with or without the membrane technique. 37,49,92However, the decision to use this technique is also strongly determined by the position of the smile line, which may require further grafting to adapt the gingival contour of the adjacent teeth and contour of the peri-implant soft tissue according to the overall esthetic situation. 43The decision about whether implant placement should be performed simultaneously with grafting or after the consolidation of the graft depends on the morphology of the defect and whether the implant can be placed within the jaw contours (see Chapter 4). Bone spreading can play an important role in preserving and expanding the remaining bone by stretching the bone walls of the future implant site, augmenting the chance of implant insertion inside the bony contour. 62If these conditions are not met, it is recommended to first carry out the grafting, and then to insert the implant after 3 months.
 In the case of an alveolar ridge width of 3 to 6 mm, the alveolar ridge can be augmented in the maxilla with extension plasty or bone splitting. This may be simultaneous or staged, depending on the stability of the vestibular mobilized bone wall. The decision to insert the implant simultaneously also depends on the possibility of inserting the implant inside the bony contours, but in addition, the implant direction must remain inside the tooth contour, which is not so easy with the bone splitting technique. For this reason, it is recommended to always combine bone splitting with a spreading of the palatal bone wall to enable the implant direction to be kept inside the tooth contour and to prevent later bone resorption and recession of the vestibular gingiva.
In the case of an alveolar ridge width of 3 to 6 mm, the alveolar ridge can be augmented in the maxilla with extension plasty or bone splitting. This may be simultaneous or staged, depending on the stability of the vestibular mobilized bone wall. The decision to insert the implant simultaneously also depends on the possibility of inserting the implant inside the bony contours, but in addition, the implant direction must remain inside the tooth contour, which is not so easy with the bone splitting technique. For this reason, it is recommended to always combine bone splitting with a spreading of the palatal bone wall to enable the implant direction to be kept inside the tooth contour and to prevent later bone resorption and recession of the vestibular gingiva.
 If the buccal bone wall becomes very mobile and thinner than 2 mm during this procedure, it is advisable to denude it from the periosteum and to stabilize the buccal wall with a bone block graft. This procedure is much more difficult in the mandible due to the cortical bone quality offering less elasticity for a greenstick fracture.
If the buccal bone wall becomes very mobile and thinner than 2 mm during this procedure, it is advisable to denude it from the periosteum and to stabilize the buccal wall with a bone block graft. This procedure is much more difficult in the mandible due to the cortical bone quality offering less elasticity for a greenstick fracture.
 A ridge width narrower than 3 mm presents an indication for a two-stage procedure. In this situation, a bone block harvested mostly from the retromolar area of the mandible is grafted to the atrophied crest following the split bone block (SBB) technique (see Chapter 4) in order to achieve long-term predictable and stable osseointegration of the implants. The implants are usually inserted 3 months after the grafting procedure.
A ridge width narrower than 3 mm presents an indication for a two-stage procedure. In this situation, a bone block harvested mostly from the retromolar area of the mandible is grafted to the atrophied crest following the split bone block (SBB) technique (see Chapter 4) in order to achieve long-term predictable and stable osseointegration of the implants. The implants are usually inserted 3 months after the grafting procedure.
2.5.1.2 Vertical bone defects
The treatment of vertical bone defects is more complicated than that of horizontal bone atrophy because they are mostly 3D defects related to severe infections, traumata, or hypodontia. Advanced atrophy or severe bone defects cause not only a loss of alveolar bone height but also an alteration in the relation of the jaws to the antagonist dentition and the occlusion. Therefore, the planning of alveolar ridge reconstruction requires consideration of the altered anatomy and the desired prosthetic result.
In the presence of insufficient bone height of < 10 mm, the following procedures are recommended:
 In the esthetic region, especially the anterior tooth area, the bone level of the neighboring teeth must be taken into consideration when planning. In principle, it is possible to augment the bone vertically only until the level of the bone covering the neighboring roots. In the situation where the bone of the neighboring teeth is partly missing, a decision must be taken with the patient about whether to accept pink ceramic in the definitive restoration or whether to remove the neighboring teeth with the missing alveolar bone before the bone grafting procedure. In cases where the neighboring teeth present sufficient bone that covers their roots, a 3D vertical bone grafting procedure following the SBB technique can be planned, since the vertical defects are normally 3D defects (horizontal and vertical). This 3D bone reconstruction can mostly be performed – up to missing vertical bone for six teeth in the anterior tooth area – with intraoral harvested bone blocks from the mandibular retromolar area. Bone grafts from extraoral sites, e.g. from the iliac crest, are used in cases where there is insufficient bone volume for the grafting procedure at the intraoral donor sites.
In the esthetic region, especially the anterior tooth area, the bone level of the neighboring teeth must be taken into consideration when planning. In principle, it is possible to augment the bone vertically only until the level of the bone covering the neighboring roots. In the situation where the bone of the neighboring teeth is partly missing, a decision must be taken with the patient about whether to accept pink ceramic in the definitive restoration or whether to remove the neighboring teeth with the missing alveolar bone before the bone grafting procedure. In cases where the neighboring teeth present sufficient bone that covers their roots, a 3D vertical bone grafting procedure following the SBB technique can be planned, since the vertical defects are normally 3D defects (horizontal and vertical). This 3D bone reconstruction can mostly be performed – up to missing vertical bone for six teeth in the anterior tooth area – with intraoral harvested bone blocks from the mandibular retromolar area. Bone grafts from extraoral sites, e.g. from the iliac crest, are used in cases where there is insufficient bone volume for the grafting procedure at the intraoral donor sites.
Читать дальше






 In the case of a partly bony defect on the vestibular and or palatal/lingual bone wall by a remaining crestal bone width of > 6 mm, implants can be inserted in combination with bone grafting using local bone chips and bone cores collected during implant preparation, with or without the membrane technique. 37,49,92However, the decision to use this technique is also strongly determined by the position of the smile line, which may require further grafting to adapt the gingival contour of the adjacent teeth and contour of the peri-implant soft tissue according to the overall esthetic situation. 43The decision about whether implant placement should be performed simultaneously with grafting or after the consolidation of the graft depends on the morphology of the defect and whether the implant can be placed within the jaw contours (see Chapter 4). Bone spreading can play an important role in preserving and expanding the remaining bone by stretching the bone walls of the future implant site, augmenting the chance of implant insertion inside the bony contour. 62If these conditions are not met, it is recommended to first carry out the grafting, and then to insert the implant after 3 months.
In the case of a partly bony defect on the vestibular and or palatal/lingual bone wall by a remaining crestal bone width of > 6 mm, implants can be inserted in combination with bone grafting using local bone chips and bone cores collected during implant preparation, with or without the membrane technique. 37,49,92However, the decision to use this technique is also strongly determined by the position of the smile line, which may require further grafting to adapt the gingival contour of the adjacent teeth and contour of the peri-implant soft tissue according to the overall esthetic situation. 43The decision about whether implant placement should be performed simultaneously with grafting or after the consolidation of the graft depends on the morphology of the defect and whether the implant can be placed within the jaw contours (see Chapter 4). Bone spreading can play an important role in preserving and expanding the remaining bone by stretching the bone walls of the future implant site, augmenting the chance of implant insertion inside the bony contour. 62If these conditions are not met, it is recommended to first carry out the grafting, and then to insert the implant after 3 months.










