Figure 9.6. Splenomegaly with spleen extending to urinary bladder. This severely enlarged spleen extends caudally to the fluid‐filled (anechoic) urinary bladder. Although it appears relatively normal regarding its echotexture and echogenicity, this dog had splenic lymphosarcoma diagnosed by percutaneous needle biopsy. Compare to Figure 9.14showing the ultrasonographic variability of splenic lymphosarcoma (LSA).
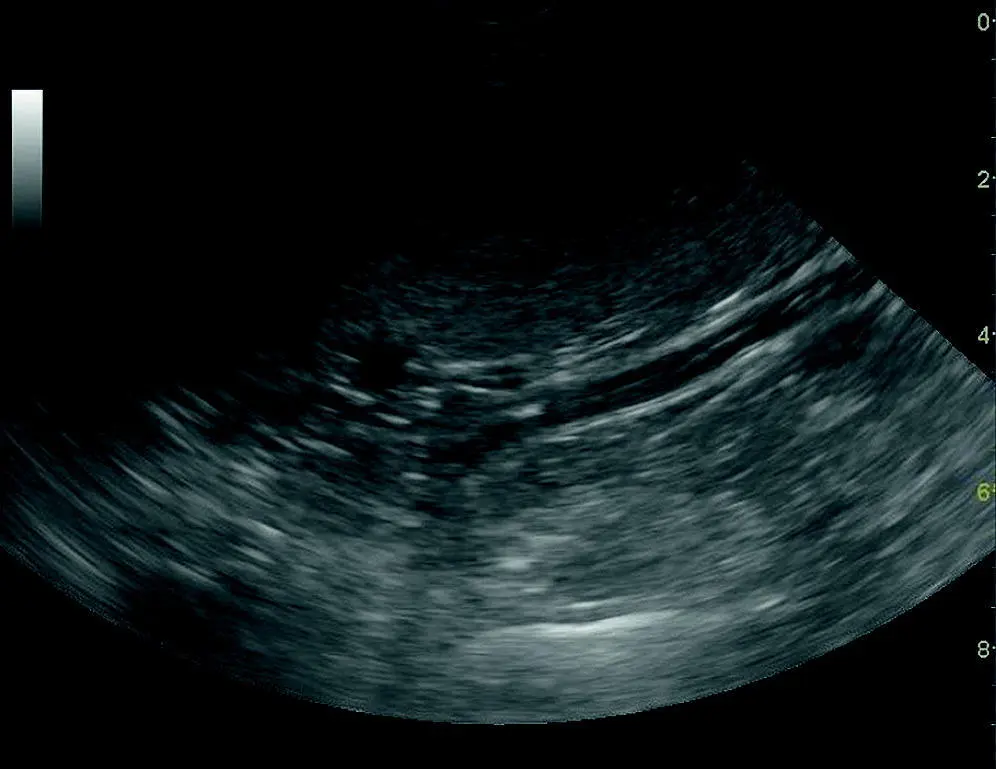
Figure 9.7. Splenomegaly with normal echogenicity. Infectious diseases can cause splenomegaly with variable changes in echogenicity. Shown here is an image from a dog with ehrlichiosis.
Pearl:In cases with nodular lesions, it may be difficult to differentiate changes associated with nodular hyperplasia from other processes without further testing (cytology or histopathology).
Myelolipoma. Myelolipomas are incidental findings in older dogs and are identified as discrete, strongly hyperechoic (bright) and frequently irregularly shaped nodules most often located near the hilus or associated with the parenchymal vessels. Less commonly, they are smooth in shape and buried within the splenic parenchyma. They are generally small in size but are occasionally quite large and can also be seen in cats. Myelolipomas are typically of no clinical consequence (incidental finding) (see Figure 9.10C,D).
Hematoma. Abdominal trauma may be associated with hematomas and splenic parenchymal injury ( Figure 9.11). Hematomas (benign masses) may be variable in appearance but initially are generally anechoic to hypoechoic (darker) when compared to normal splenic parenchyma. As the blood within the hematoma forms a clot, the lesion may become more isoechoic or hyperechoic to normal parenchyma. As the clot retracts, the lesion may again become hypoechoic. Anechoic fluid may form around the clot and appear as a cyst‐like lesion. These factors may make hematomas difficult to distinguish from other mass lesions, including neoplasia.
Pearl:Fine needle biopsy of hematomas generally yields nonspecific cytological results and therefore the absence of neoplastic cells on cytology does not rule out neoplasia. A more definitive diagnosis of hematoma is obtained by splenectomy and histopathological evaluation; however, even this may be complicated by a large hematoma associated with a smaller malignant mass, resulting in a possible misdiagnosis.
Abscess. Splenic abscesses are uncommon and usually cannot be distinguished from other processes that produce nodular or mass lesions. The appearance may be variable with well‐defined or indistinct margins and variable echogenicity. Abscesses most commonly appear as hypoechoic lesions, which may have cystic components or mixed echogenicity. A more conclusive finding for an abscess (in contrast to neoplastic processes) is the presence of gas (due to gas‐forming bacteria) within the lesion. This appears as focal areas of hyperechogenicity with distal edge shadowing (see Chapter 3).
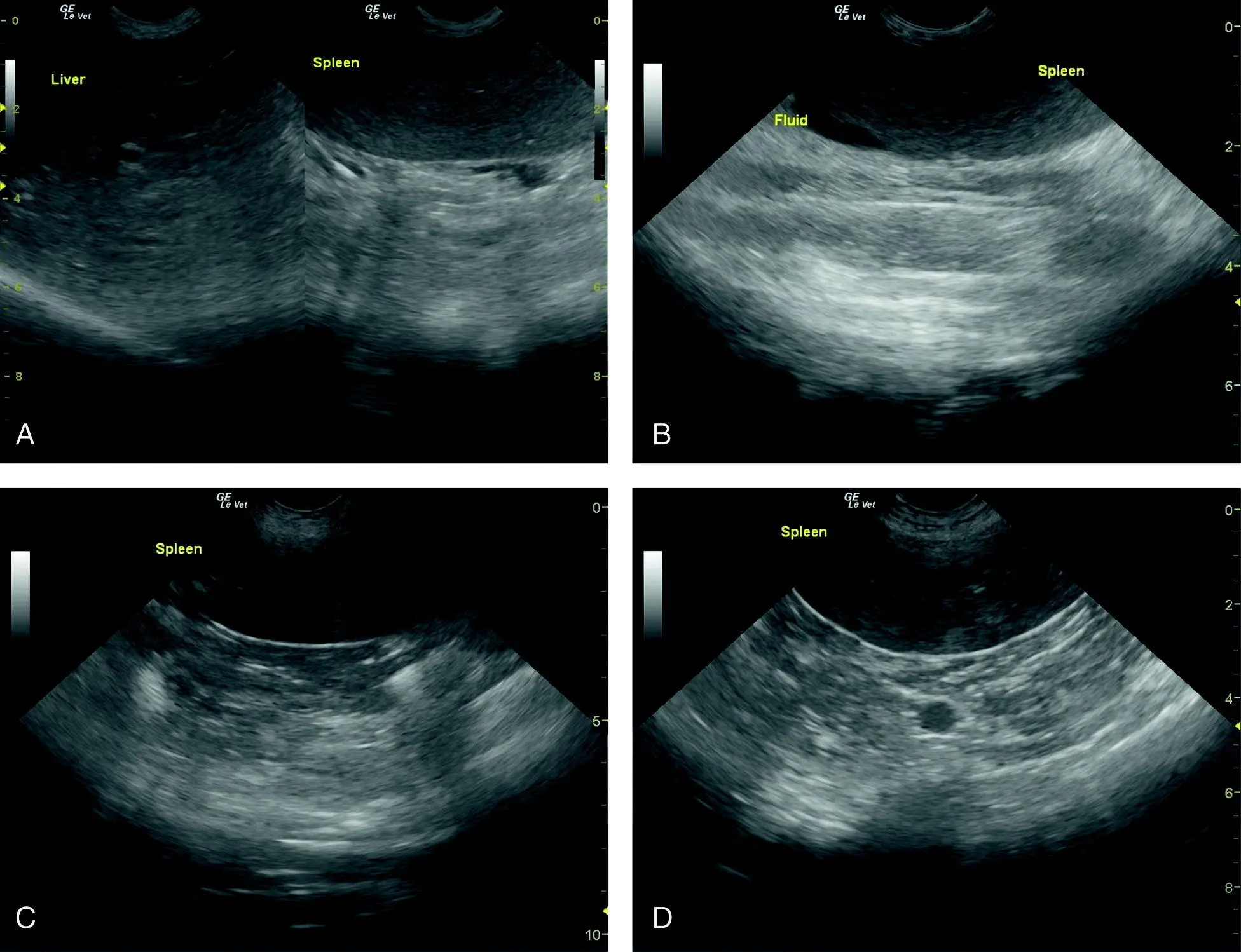
Figure 9.8. Splenomegaly with splenic hyperechogenicity (brighter than normal) and hypoechogenicity (darker than normal). (A) Relatively normal homogeneous echotexture in a hyperechoic (brighter than the liver) spleen. The diagnosis by percutaneous needle biopsy was lymphosarcoma (LSA). (B) Another relatively unremarkable hyperechoic spleen in a cat diagnosed with splenic LSA by percutaneous needle biopsy. Note an anechoic triangle of free fluid (Fluid). (C,D) Mottled echotexture with hypoechogenicity (darker) in spleens representing nodular hyperplasia diagnosed by percutaneous needle biopsy.
Pearl:Fine needle aspiration/needle biopsy with cytology and bacterial culture and sensitivity is helpful in confirming a splenic abscess diagnosis. Be aware that necrotic centers of neoplastic lesions can be mistaken for abscesses, and so diagnosis should always be in conjunction with clinical findings and in some cases a definitive diagnosis may only be gained with splenectomy and histopathological evaluation.
Splenic neoplastic lesions can have a wide range of ultrasonographic changes. As emphasized above, it is not possible to distinguish between benign and malignant lesions based on ultrasonographic appearance alone. The most common types of splenic neoplasia found in dogs are hemangiosarcoma and lymphosarcoma (Hecht 2008) but other primary and metastatic tumors are possible.
Hemangiosarcoma (HSA) generally appears as complex mass lesions with mixed echogenicity and cavitations that distort the splenic capsule ( Figure 9.12). HSA of the spleen is often associated with acute or chronic hemorrhage, and animals with ruptured splenic masses causing hemoabdomen have a higher likelihood of malignancy (hemangiosarcoma) (Hammond and Pesillo‐Crosby 2008). Definitive preoperative diagnosis of HSA is challenging, however, since rupture of splenic masses with resultant hemoabdomen can occur with both benign and malignant processes, and since benign hematomas and HSA can have similar ultrasonographic appearances. The presence of suspected metastatic nodules elsewhere in the abdomen or thorax increases the index of suspicion for malignancy, but a definitive diagnosis is often not made without splenectomy and histopathology, and even then can be complicated by an associated hematoma.
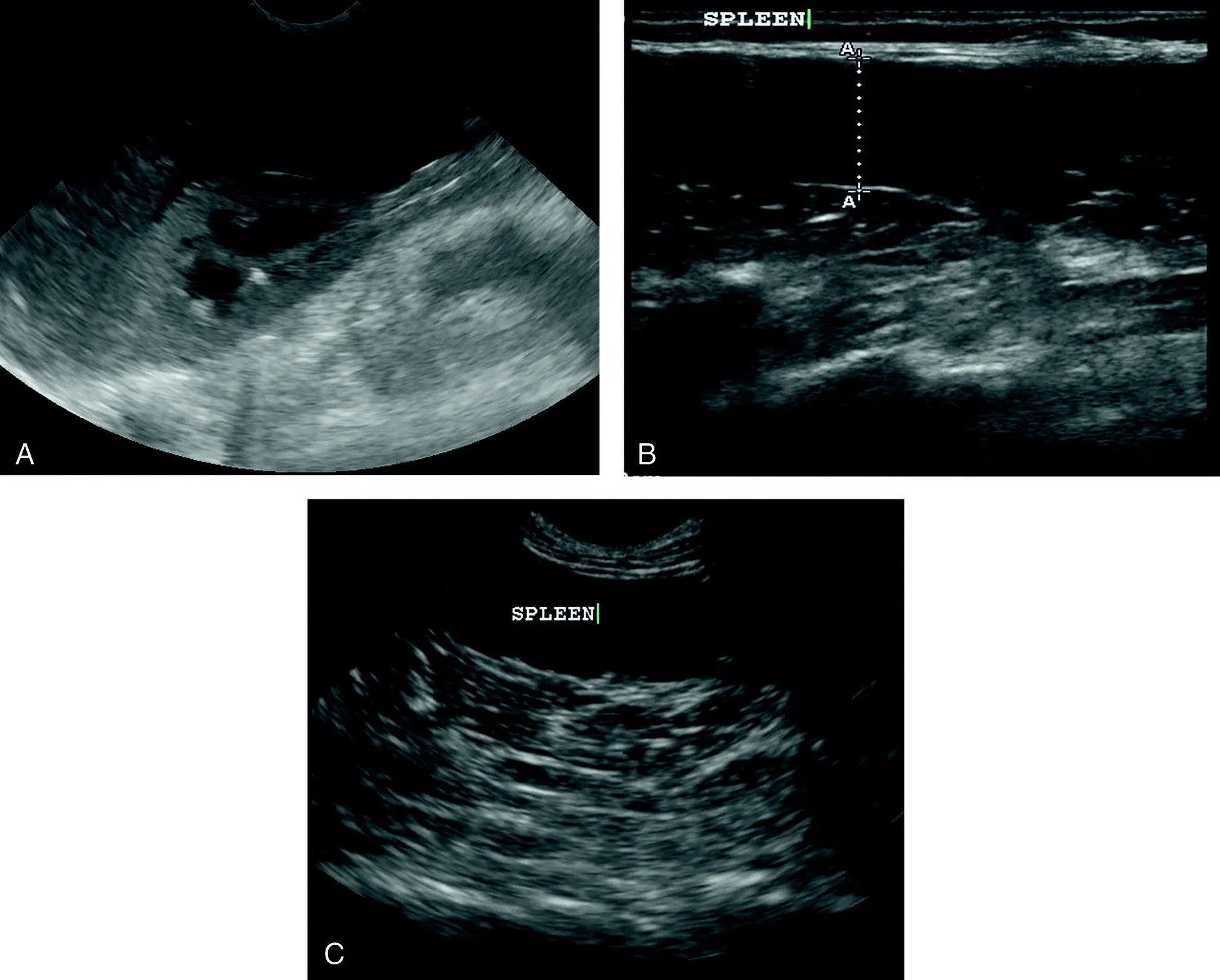
Figure 9.9. Splenomegaly with splenic hypoechogenicity (darker than normal). (A) Comparative echogenicity of the spleen to the cortex of the left kidney. Suppurative splenitis was diagnosed by percutaneous needle biopsy. (B) Splenomegaly determined by a splenic thickness that was >10 mm (measured by calipers marked “A”) with concurrent hypoechogenicity (darker) in a cat. Histoplasmosis was diagnosed by percutaneous needle biopsy. (C) Diffuse parenchymal changes not much different from (A) and (B) diagnosed by percutaneous needle biopsy as mast cell tumor. These examples illustrate that clinical diagnosis cannot be made based on ultrasonographic appearance alone.
Pearl:Staging of HSA may be assisted by performing a Global FAST to evaluate for hemoabdomen (AFAST), pericardial effusion (and right atrial mass) and Vet BLUE lung ultrasound for pulmonary metastasis.
Metastatic lesions may be hypoechoic or hyperechoic in nature and are more likely to have a “target” appearance consisting of hypoechoic margins with a relatively hyperechoic center ( Figure 9.13). Single target lesions have a high predictive value for malignancy and when multiple target lesions are seen, the positive predictive value of malignancy increases from 74% to 81% (Cuccovillo and Lamb 2002). One must keep in mind, though, that a sonographic target lesion is a nonspecific finding and a biopsy is required for diagnosis. When finding a splenic target lesion, look for other intraabdominal or intrathoracic masses using Global FAST, radiography (screening for lung nodules) or both. The identification of additional nodules provides further suspicion for malignancy and may also provide a more accessible scanning plane for percutaneous sampling. Figure 9.10.Splenic nodular hyperplasia and myelolipomas. (A–C) Examples of nodular hyperplasia characterized by homogeneous echogenicity of the mass which may be hyper‐ or hypoechoic relative to the adjacent splenic parenchyma. Importantly, note that in contrast to fluid‐filled structures that have acoustic shadowing artifact extending through their far‐field, these solid nodules do not. Also, in the distal field is a transverse image of normal small bowel that appears like a “hamburger” (colored cartoon to the lower right of the small bowel). (D) An example of a myelolipoma, a common incidental finding in older dogs, often hyperechoic (bright) discreet nodules located near the splenic hilus but may also be located parenchymally. Figure 9.11.Splenic hematomas and infarcts. (A) The spleen has a hypoechoic (dark) area within its parenchyma that represents an acute hematoma in a young dog that had just incurred blunt automobile trauma. The splenic finding was observed during an AFAST exam. (B) The spleen has a hypoechoic area within its parenchyma that represents an infarcted region seen in a bluntly traumatized puppy.Source: (B) courtesy of Dr Autumn Davidson and Tomas Baker, University of California, Davis, CA. Figure 9.12.Splenic hemangiosarcoma (HSA) and its variability. (A) A splenic mass that was diagnosed as HSA by splenectomy and histopathological evaluation. Note normal spleen in the upper left image is confluent with the mass of mixed echogenicity determining its splenic origin. (B,C) Typical mass appearances of splenic HSA. For positive splenic identification, the mass should be traced into obvious splenic parenchyma. Surprisingly, in some cases, HSA and other splenic masses can mimic the less common benign diagnosis of splenic abscess. A large splenic mass of mixed echogenicity or with a necrotic center may also mimic free fluid when depth is inadequate (too zoomed in or the depth set too shallow) or the mass is excessively large (exceeding the depth limits of your ultrasound machine). (D) An example of HSA that is more infiltrative and less mass‐like. Note that despite the mixed echogenicity, the spleen has little to no deformation of its normal contour.
Читать дальше