This book has been written out of a passion to explain in simple terms ‘everything you really need to know but no‐one told you’ about the recognition and management of a sick adult. Unlike most medical books, this one does not give you a list of things to do, nor does it bore you with small print. This book helps you understand what you need to do and why . The second edition has been extensively rewritten and updated, with algorithms and references in a clear, simple format. The authors are medical educators as well as busy clinicians who envisage that the book will be used by teachers as well as learners. I recommend it highly.
Alastair McGowan OBE FRCPE FRCP FRCS FRCA FCEM
Consultant in Emergency Medicine
Past President of the Faculty of Accident and Emergency Medicine, UK
Standard international (SI) units are used throughout this book, with metric units in brackets where these differ. Below are some reference ranges for common blood results. Reference ranges vary from lab to lab.
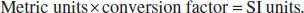
| Test |
Metric units |
Conversion factor |
SI units |
| Sodium |
135–145 meq/L |
1 |
135–145 mmol/L |
| Potassium |
3.5–5.0 meq/L |
1 |
3.5–5.0 mmol/L |
| Urea (blood urea nitrogen) |
8–20 mg/dL |
0.36 |
2.9–7.1 mmol/L |
| Creatinine |
0.6–1.2 mg/dL |
83.3 |
50–100 μmol/L |
| Glucose |
60–115 mg/dL |
0.06 |
3.3–6.3 mmol/L |
| Partial pressure O 2 |
83–108 mmHg |
0.13 |
11–14.36 kPa |
| Partial pressure CO 2 |
32–48 mmHg |
0.13 |
4.26–6.38 kPa |
| Bicarbonate |
22–28 meq/L |
1 |
22–28 mmol/L |
| Calcium |
8.5–10.5 mg/dL |
0.25 |
2.1–2.6 mmol/L |
| Chloride |
98–107 meq/L |
1 |
98–107 mmol/L |
| Lactate |
0.5–2.0 meq/L |
1 |
0.5–2.0 mmol/L |
ACC/AHAAmerican College of Cardiology and American Heart AssociationACTHAdrenocorticotropic hormoneADHAnti‐diuretic hormoneAFAtrial fibrillationAKIAcute kidney injuryALIAcute lung injuryAMPAdenosine monophosphateANCAAnti‐neutrophil cytoplasmic antibodiesAPACHEAcute physiological and chronic health evaluationAQPAquaporin receptorARBsAngiotensin‐receptor blockersARDSAcute respiratory distress syndromeASAortic stenosisASAAmerican Society of AnesthesiologistsASA‐PSASA Physical StatusASBAssisted spontaneous breathsATAnaerobic thresholdATLSAdvanced Trauma and Life SupportATPAdenosine triphosphateAVPUalert, responds to voice, responds to pain, unresponsiveBEBase excessBiPAPBilevel positive airway pressureBPBlood pressureBPSBehavioural Pain ScaleBTSBritish Thoracic SocietyBUPABritish United Provident AssociationCBFCerebral blood flowCGAComprehensive geriatric assessmentCKCreatine kinaseCKDChronic kidney diseaseCOCarbon monoxideCOCardiac outputCOPDChronic obstructive pulmonary diseaseCPAPContinuous positive airway pressureCPPCerebral perfusion pressureCPRCardio‐pulmonary resuscitationCPXCardiopulmonary exerciseCRPC‐reactive proteinCTComputed tomographyCVPCentral venous pressureCVPUConfused, responds to voice, responds to pain, unresponsiveCVRCerebrovascular resistanceECGElectrocardiogramECMOExtracorporeal membrane oxygenationeGFREstimated glomerular filtration rateEPAPExpiratory pressureERASEnhanced Recovery After SurgeryERCPEndoscopic retrograde cholangio‐pancreatogramFASFunctional Activity ScoreFDAFood and Drug AdministrationFLACCFaces Legs Activity Cry ConsolabilityFVCForced vital capacityGBMGlomerular basement membraneGCSGlasgow Coma ScoreGPGeneral practitionerHASHuman albumin solutionHESHydroxyethyl starchHFmrEFHeart failure with mid‐range ejection fractionHFNOTHigh flow nasal oxygen therapyHFpEFHeart failure with a preserved ejection fractionHFrEFHeart failure with reduced ejection fractionHRHeart rateIASPInternational Association for the Study of PainICPIntracranial pressureIPAPInspiratory pressureIPPVIntermittent positive pressure ventilationIVCInferior vena cavaKDIGOKidney Disease Improving Global OutcomesLALeft atriumLEDsLight emitting diodesLPLumbar punctureLRINECLab Risk Indicator for Necrotising FasciitisLVEFLeft ventricular ejection fractionLVHLeft ventricular hypertrophyMACEMajor adverse cardiac eventsMAPMean arterial pressureMETsMedical emergency teamsMETsMetabolic equivalentsMRIMagnetic resonance imagingNCEPODNational Confidential Enquiry into Patient Outcome and DeathNEWS2National Early Warning ScoreNICENational Institute for Health and Care ExcellenceNIVNon‐invasive ventilationNSAIDsNon‐steroidal anti‐inflammatory drugsOSAObstructive sleep apnoeaPAPulmonary arteryPAMPsPathogen‐associated molecular patternsPCIPercutaneous coronary interventionPEEPPositive end‐expiratory pressurePOCUSPoint of care ultrasoundPOISEPerioperative ischaemic evaluationPOSSUMPhysiological and operative severity score for the enumeration of mortality and morbidityPSVPressure support ventilationqSOFAQuick SOFASA‐AKISepsis associated acute kidney injurySAFESaline vs. albumin evaluationSAHSubarachnoid haemorrhageSAHLSepsis‐associated hyperlactateaemiaSIMVSynchronised intermittent mandatory ventilationSIRSSystemic inflammatory response syndromeSOFASepsis‐related organ failure assessmentSORTSurgical Outcome Risk ToolSRSSurgical Risk ScaleSSCSurviving Sepsis CampaignSVStroke volumeSVRSystemic vascular resistanceTENSTranscutaneous nerve stimulationTHRIVETransnasal humidified rapid insufflation ventilatory exchangeTLRsToll‐like receptorsTTPThrombotic thrombocytopenic purpuraVANISHVasopressin versus Norepinephrine as Initial Therapy in Septic Shock TrialVASSTVasopressin and Septic Shock TrialVILIVentilator‐induced lung injury
CHAPTER 1 Patients at Risk
By the end of this chapter you will be able to:
Define resuscitation
Recognise the importance of the generic altered physiology that accompanies acute illness
Know that early recognition and management improves outcomes
Know how to assess and manage an acutely ill patient using the ABCDE system
Understand the benefits and limitations of intensive care
Know how to communicate effectively with colleagues about acutely ill patients
Have a context for the chapters that follow
When we talk about ‘resuscitation’ we often think of cardio‐pulmonary resuscitation (CPR). CPR is a significant part of healthcare training. International organisations govern resuscitation protocols. Yet, survival to discharge after in‐hospital CPR is poor, around 50% if the rhythm is shockable and 10–14% if the rhythm is non‐shockable. 1Public perception of CPR is often informed by television which has far better outcomes than in reality. 2
A great deal of attention and training is focussed on saving life after cardiac arrest. But the majority of in‐hospital cardiac arrests are predictable and preventable. Until the last few decades, hardly any attention was focussed on detecting commonplace reversible physiological deterioration and in preventing cardiac arrest in the first place. Now, we have early warning scores and medical emergency teams – but there still remain problems with the early recognition and management of sick patients in hospital.
In a study published in 1990, 84% of patients had documented observations of clinical deterioration or new complaints within 8 hours of cardio‐pulmonary arrest and 70% had either deterioration in respiratory or mental function observed during this time. 3While there did not appear to be any single reproducible warning signs, the average respiratory rate of the patients prior to arrest was 30/min. The investigators observed that the predominantly respiratory and metabolic derangements which preceded cardiac arrest (hypoxaemia, hypotension, and acidosis) were not rapidly fatal and that efforts to predict and prevent arrest would therefore be beneficial. Only 8% patients survived to discharge after CPR. A subsequent similar study observed that documented physiological deterioration occurred within 6 hours in 66% of patients with cardiac arrest, but effective action was often not taken. 4
Читать дальше